Diseases & Conditions, Featured, Veterinary
Wet skin conditions in horses
Stuart Davies looks at the causes, diagnosis and treatment of mud fever, rain scald and other wet skin conditions in horses
The mild climate in the UK brings us cool and wet winters – a combination that leads to the increase in skin infections we usually see in the winter months. So, we are going to look at which infections occur, how they can be treated and, how we can prevent them!
The skin is both an anatomical and a physiological barrier that protects the horse from the external environment. It is considered the largest organ of the body and its function not only reflects its own health but also, that of various organ systems. It is composed of several layers of cells, sweat glands and hair follicles. Anatomically its thickness and the destiny of hair coverage reduces from the horse’s back, down to the bottom of its legs – the hair growing cycle is also affected by the general health of the horse.
Melanin, the pigment within human skin, is also present in horses. It has a protective function by absorbing ultraviolet radiation emitted by the sun and removing free radicals, which cause tissue damage. In areas where melanin is lacking such as pink skinned muzzles and legs, the immune system function of the skin is impaired. This, in combination with thinner skin and hair coverage, leads to an increased risk of skin disease affecting these areas¹.
Skin disease is often progressive. This means that there can be a cross over between the clinical signs of numerous different skin diseases – depending at which stage the horse is presented. Clinical signs of a skin infection include the appearance of inflamed skin; redness, heat, swelling and sometimes discomfort when the area is touched. The hair growth cycle is usually halted leading to alopecia (hair loss). Excessive scales may be present when the health of the skin is compromised.
Papules and pustules are liquid containing swellings, that are differentiated based on size. Once open, the fluid becomes dried and forms a crust. Bacterial infections of the skin tend to be caused by the Staphylococcus species – these bacteria can be found on the skin of healthy horses and, are classed as an ‘opportunistic’ species, meaning that it takes advantage when environmental factors allow². There is a particular concern regarding its ability to transfer resistant genes between each other, which poses a risk of resistance for the use of antibiotics in both the veterinary and human medical world³.
Skin infections vary in how itchy or ‘pruritic’ the horse becomes and they are not seen only in winter but, can occur in areas where the tack sits during warmer summer months, when sweat is not washed adequately out of the coat.
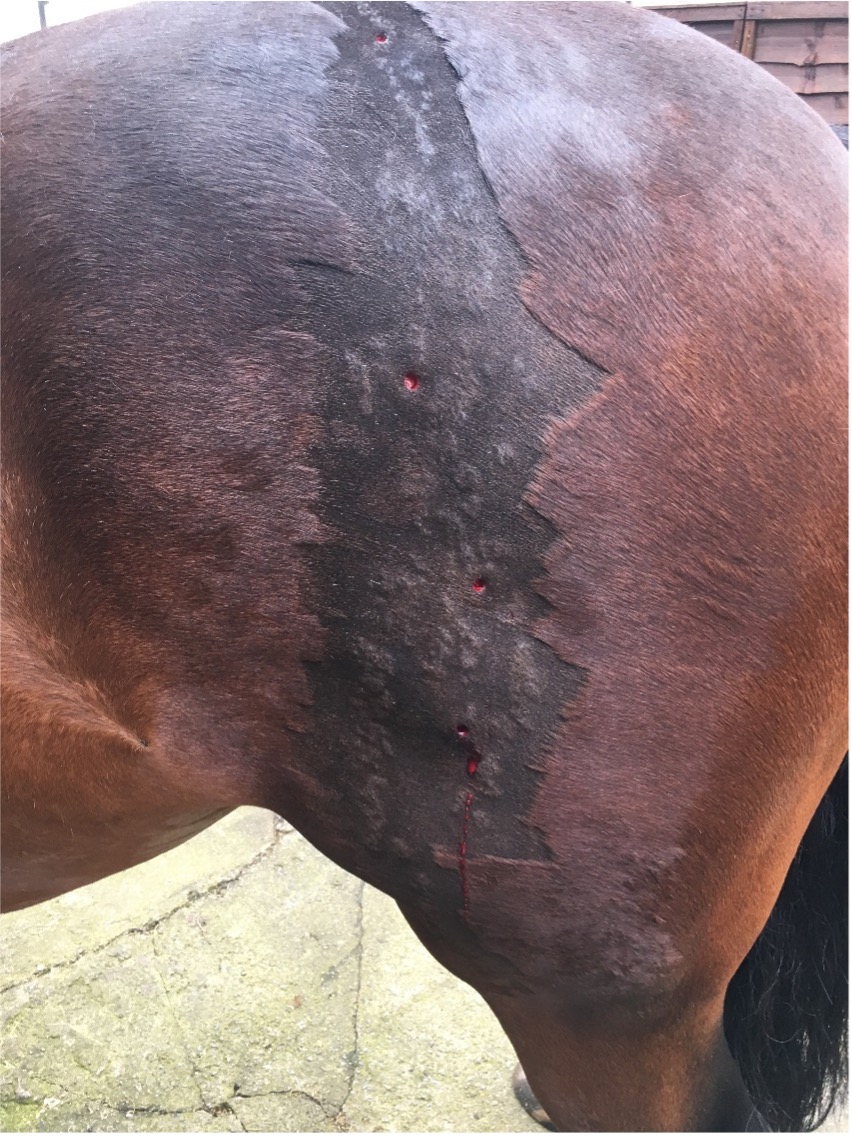
Rain scald
Rain scald is a skin infection caused by another bacterium, Dermatophilus congolensis. Thick adherent hair plaques lead to alopecia and, underlying inflamed skin in areas that are chronically wet. Therefore, this often occurs on the backs of unrugged or, inadequately rugged horses out at pasture. Interestingly under a microscope this bacterium forms chains, making easy to diagnose.
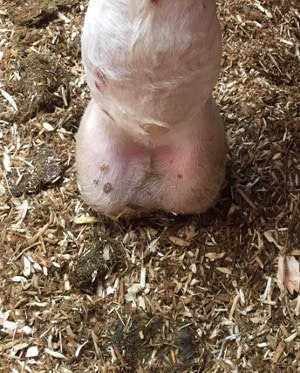
Mud fever
Mud fever, greasy heel, cracked heel – the list goes on, are various colloquial terms for pastern dermatitis. While it doesn’t exclusively occur in the winter, wet conditions appear to increase its prevalence. Various bacteria have been cultured from lesions, which is most probably due to the proximity to the ground and exposure to dirt and faeces.
Lesions are usually restricted to the back of the pastern but, can extend to affect the fetlock and canon. These usually present as scabs, worsening into larger areas of exudative (producing a discharge) lesions, becoming very sore to touch and, with associated limb swelling. Left untreated this can have serious consequences, with progression to limb cellulitis/ lymphangitis and long-lasting damage to the lymphatic system of the limb, with an increased risk long term of recurring episodes.
The treatment of bacterial skin infections revolves around management in addition to topical or systemic antimicrobials. Topical antimicrobial washes most commonly used are chlorhexidine or iodine based. Various antimicrobial topical lotions/ creams or sprays are available but silver/ aluminium containing products are a particular favourite. Systemic antimicrobials licensed for use in horses are limited and ideally, should be guided by culture and sensitivity results, following responsible antimicrobial care. However, trimethoprim sulfadiazine is often a broad spectrum first line antibiotic prescribed that is suitable in most cases.
To allow successful treatment of infected areas it is often necessary to clip the hair to increase air flow, reduce moistness and heat and, allow adequate application of topical products.
Ringworm
If antimicrobial treatments fail, this may be an indication that fungal disease is present. Dermatophytosis or ringworm is a zoonotic disease so, good biosecurity and hand-washing of infected animals and humans should be undertaken to prevent transmission.
Ringworm lesions are seen usually, but not only, on the face. They classically appear as circular adherent hair plaques with surrounding crust, often described as being like ‘cigarette ash’. An increased prevalence of this disease occurs in winter, which is likely due to reduced exposure to UV and increased close contact from stabling, thick coats and rugging.
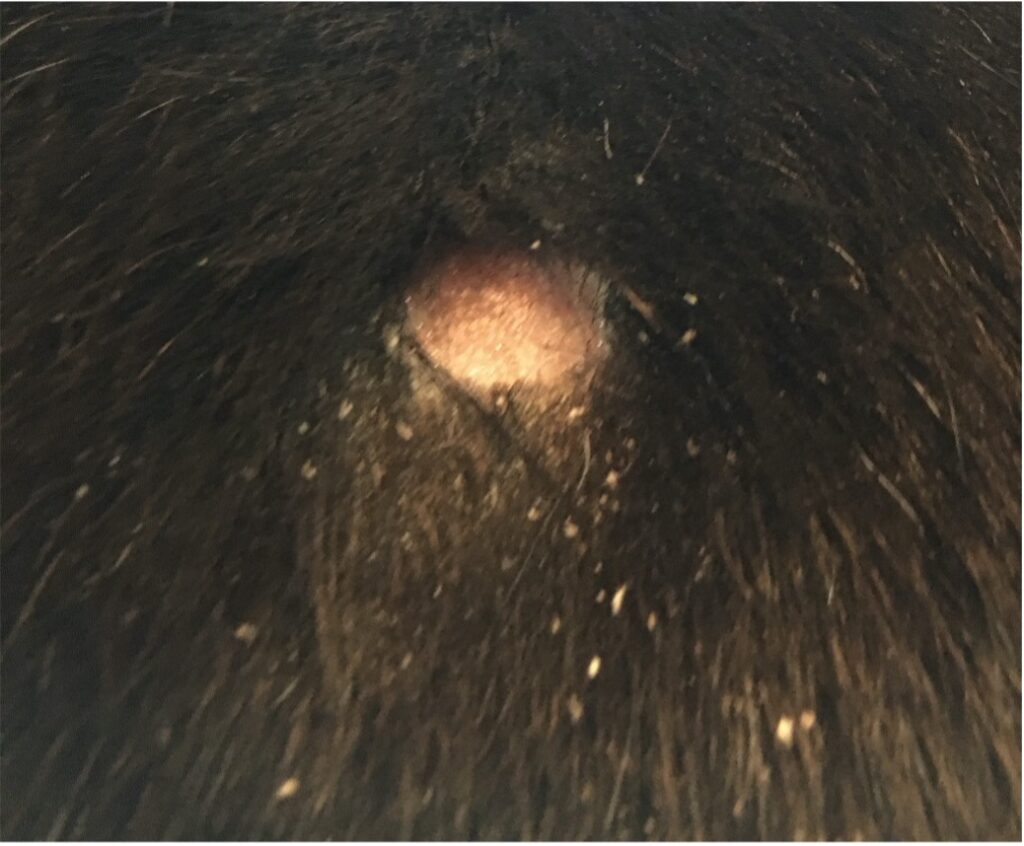
Diagnosis is made by sending a pluck of hair, or scab for a pcr test – diagnosis by polymerase chain reaction. This detects DNA whether dead or alive, it is very accurate and has a quick result so is the test of choice². Treatment then must be adjusted to include an appropriate topical wash, such as those containing enilconazole. Interestingly an inactivated vaccine is available and used on the continent, effective at protecting at least 80% of vaccinated horses⁵.

A yeast known as Malassezia can also be associated with a pruritic skin disease in the horse. Yeast cells can be seen as monkey nut shapes on microscopic examination of impression smears. Treatment of these infections is usually successful using a milconazole shampoo².
Recommendations to prevent skin infections
- Allow horses dry period. It is undeniable that exposing horses to wintery conditions is more natural and can have benefits for weight management by utilising energy to thermoregulate. However, a well waterproofed rug can protect areas where recurrent wetting or water can accumulate, such as on the back.
- Ensure a good grooming routine is maintained to allow the early identification of skin/ hair lesions
- Water repellent ointments can be applied to limbs
- Boots/ wraps can be used but, care must be taken to prevent abrasions from the boots themselves or dirt getting trapped adjacent to the skin
- Control any conditions causing pruritis such as chorioptes (feather mite), atopy or lice. This will prevent opportunistic infections of self-inflicted wounds If any wounds are noticed, then washing them in an antimicrobial wash such as povidine iodine or chlorhexidine prior to applying antimicrobial topical products, will be beneficial to reduce contamination. Be sure to not use the product in too strong a concentration as this can be deleterious to cells. Dilution to use is approximately 1 capful to 1 bucket.
- Leaving legs to dry and brushing off mud or, washing legs and drying gently is always a hotly debated topic. I personally prefer for them to dry as repeated wetting of the skin can reduce skin health. There has been a product called Mudstop, tested for effectiveness with some success. This is a spray combination of antimicrobial and two humectants. Humectants moisturise the scabs, meaning they don’t have to be removed but rather should drop off after a week⁴.
Related reading:
What is elephant leg, cellulitis or lymphangitis in horses? Understanding lymphangitis Help my horse has mud fever Hibiscrib – are you using it correctly
References
- White, S. D. (2005) ‘Equine Bacterial and Fungal Diseases: A Diagnostic and Therapeutic Update’, Clinical Techniques in Equine Practice, 4(4), pp. 302–310. doi: 10.1053/j.ctep.2005.10.004
- R. Yasuda, J. Kawano, H. Onda, et al. Methicillin-resistant coagulase-negative staphylococci isolated from healthy horses in Japan Am J Vet Res, 61 (2000), pp. 1451-1455
- Colles, C.M., Colles, K.M. and Galpin, J.R. (2010), Equine pastern dermatitis. Equine Veterinary Education, 22: 566-570
- A.C. Pier, P.J. Zancanella Immunization of horses against dermatophytosis caused by Trichophyton equinumEquine Pract, 15 (1993), pp. 23-27
