Diseases & Conditions
Feather mites and other itches
Stuart Davies BVSc MRCVS, advises why itches should not be ignored, and explains how an accurate diagnosis is key to successful treatment
‘Pruritis’ or the sensation to itch is a common occurrence in equine practice and can be frustrating for both horse and owner. In severe cases horses will cause injury to themselves as well as to their surroundings to gain satisfaction. The location on the body and the season when itchiness becomes apparent can be pathognomic for certain causes of pruritis. However, it can also be necessary to have veterinary involvement to achieve a diagnosis in order to correctly target treatment and prevention.
There are many different parasitic causes of pruritis, and these are often the first cause to be eliminated when presented with a case.

Chorioptes equi
Often termed the ‘feather mite’, chorioptes equi is usually associated with biting and stamping of the lower limbs in feathered breeds. The feather mite dwells on the surface of the skin and its presence leads to serum ooze, crusting and adherence of hair within the feathers of affected animals. These changes at the back of the knee and front of hock, termed ‘malanders / salanders can make the horse particularly sensitive to palpation. Longer term infection results in lichenification, or thickened skin folds, which can then allow the mite to be hidden from topical treatments.

Figure 1. Several focal areas of pastern dermatitis, also termed mud fever. These are often a consequence of self trauma due to pruritis from Chorioptes infection
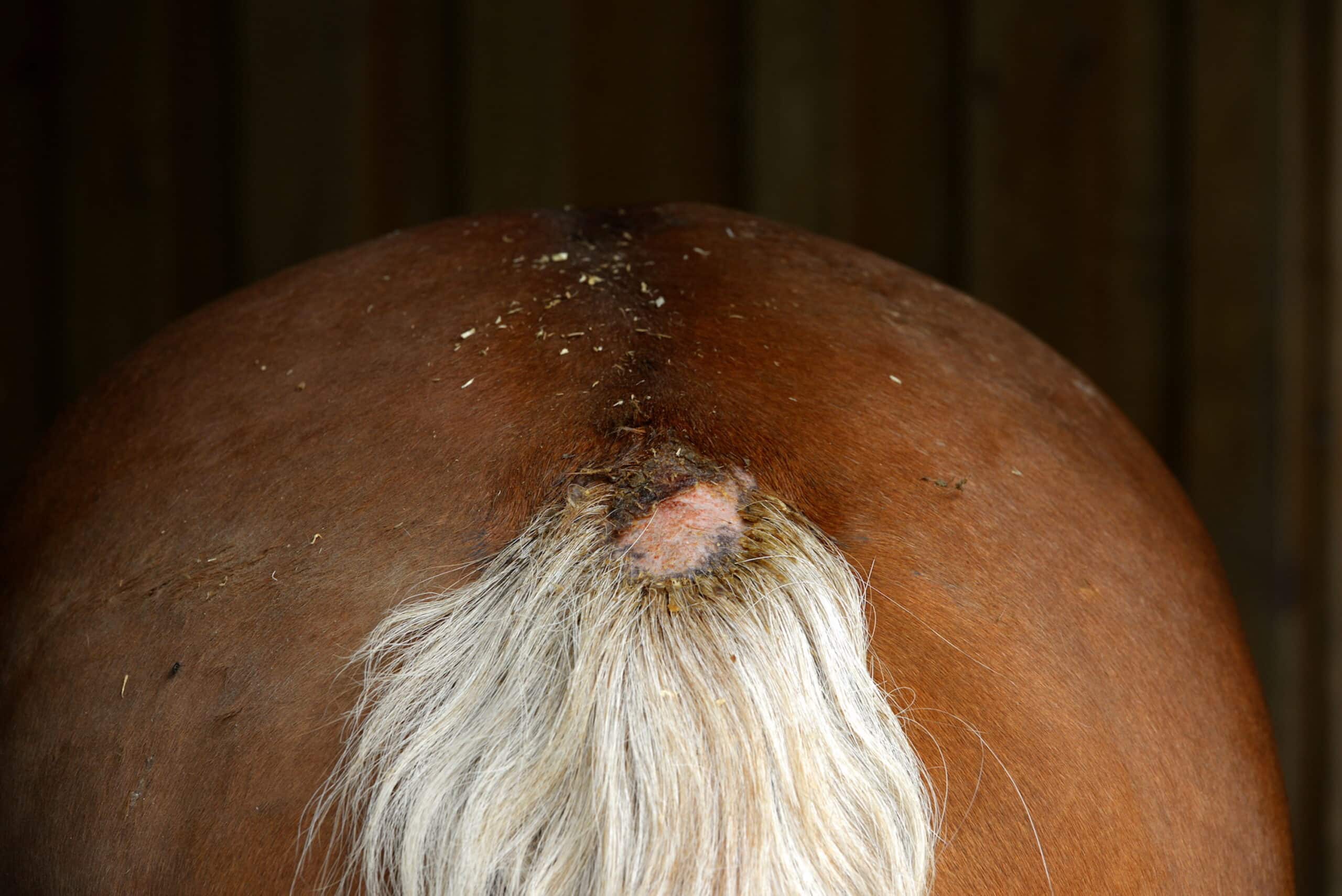
Figure 2: Alopecia (hair loss) and erythema (reddening) due to self-trauma of the tail
Despite its colloquial name the mite can actually be found on other lighter haired horses¹. It is possible that recurring infections are due to these asymptomatic carriers, if not due to the reported two-month environmental survival².
Although the presentation of chorioptes is recognisable, skin brushings can be examined under the microscope for confirmation.There is little available in terms of licensed medications to treat these cases.
However, there are some products available for other species that have been shown to be useful:
- 2% Lime Sulphur when used following leg clipping and a benzyl peroxide wash at weekly intervals eliminated mites from samples after four weeks in all horses². Benzyl peroxide breaks down adherent scabs and reduces the exudation from the skin².
- Selenium Sulphide shampooing three times over 15 days removed all mites and signs of disease in one study. The mode of action of sulphurous based shampoos is unknown, but the act of shampooing could also be beneficial to remove crust, the food source of the mites. Sulphurous shampoos can change the colour of white hair and tend to be strongly odoured³.
- Fiprinol has been applied once to the limbs with a reduction in mite numbers and clinical signs by day 28 ⁴.
- Doramectin is an injectable product licensed for the treatment of the Chorioptes mite in cattle and sheep. It has been shown to reduce mite numbers and clinical signs in 28 days after two injections 14 days apart. Recently a topical formulation of this drug has become available to the market, with no studies to show effectiveness currently ⁵.
- Environmental disinfection is usually incorporated into treatment. This can be difficult, and disinfectants used are usually those that are shown to destroy worm eggs.
- Clipping can be met with reluctance. However, thick hair can prevent topical applications from reaching the skin and protect mites from environmental conditions. Removal of hair may also benefit from removal of mites and crust itself.
Anecdotally, not every treatment works 100% for every patient. Signs usually recur after 6 months and repeat treatments are often necessary. Note: many of the above treatments are POM-V so it is advisable to seek veterinary guidance.
Dermanyssus gallinae⁶, the poultry red mite, and Trombicula Autumnalis, the harvest mite, less commonly cause pruritis in the horse. These are visible to the eye, are coloured red and orange respectively and, may be found in other areas of the body¹.
Lice
Infestations of lice can occur in healthy individuals⁷ as well as those with suppressed immune systems, such as youngsters or, elderly horses with pituitary pars intermedia dysfunction. Two different species can affect horses W. equi, a biting louse, and H.asini, a sucking louse. As well as causing pruritis, patchy alopecia (hair loss) and a peeling appearance to the skin are pathognomic⁸. H. asini usually is found under the mane and W.equi on the body⁹.
 Lice are typically a winter problem and can be visualised as yellow/ brown wingless insects while their eggs are yellow, 1 mm in size and adhered to the hairbase. The life cycle lasts between 10-20 days and requires the host while the eggs, ‘nits’, are viable, for 3 weeks.
Lice are typically a winter problem and can be visualised as yellow/ brown wingless insects while their eggs are yellow, 1 mm in size and adhered to the hairbase. The life cycle lasts between 10-20 days and requires the host while the eggs, ‘nits’, are viable, for 3 weeks.
As with mites, similar treatment options exist such as selenium sulphide shampoos⁹ and fipronil ⁸. Clipping is also a good way to reduce louse numbers. However, clipping as a sole method of control of louse numbers during winter months has been shown to be ineffective¹⁰. Topical permethrin-based products are the mainstay of treatment¹¹. These are usually easy to apply however have been associated with resistance development in sheep so should be used only when necessary. Treating the herd or in contact animals in addition to the environment such as rugs and grooming kits is necessary to control the lice numbers.
Oxyuris equi
Also known as pinworm, oxyuris equi was previously reported to be of minor significance in relation to disease. However, affected individuals can experience intense pruritis of the perianal area and therefore traumatise the rump and tail head. Female worms occupy the large intestine and migrate to the rectum to lay eggs in a sticky mucus on the perianal skin. These adherent eggs are responsible for the pruritic reaction. Rubbing this area on stables and fence lines can contaminate the environment and enable transmission to field mates. However, the development of infestation and appearance of clinical signs appears to be individual as not all horses kept in the same environment will exhibit clinical signs.
Resistance to anthelmintics is an increasing concern amongst endoparasite populations and, oxyuris equi can be troublesome to treat.
If you are suspicious of pinworm affecting your horse a piece of cellotape repeatedly applied to the perianal region can then be examined under a microscope for the presence of lemon shaped eggs.
Onchocerca cervicalis
Uncommon but, does occur in the UK. The larvae called microfilaria are spread via biting midges and localise in the neck where they cause a local pruritis when they die. It is an important differential for atopic skin disease and, is successfully treated with ivermectin or moxidectin anthelmintics, which may be the reaits low occurrence in the UK population¹³.
Bacterial infections
These can also be linked to a variable pruritis; in addition to swelling and discomfort typically in the saddle and lumbar area due to poor fitting tack, poor grooming or warm wet weather. These areas then develop into papules and crusts¹⁴.
Fungal infections
The most commonly encountered, dermatophytosis (ringworm) can result in variably pruritic lesions. These lesions usually present in well circumscribed crusting/ hair less lesions and is zoonotic, transmissable from horse to human. Therefore, care should be taken and, good hand hygiene to prevent inadvertent contamination. Transmission occurs between shared tack/ grooming brushes or direct contact. Treatment is curative with the owner predominantly using enilconazole solution applied to the lesions, in addition to disinfection of equipment¹⁵.
Immune mediated or hypersensivity reactions can be considered once the above has been excluded and, will be discussed in the next part of this piece on possible causes of an itchy horse.
References
- Pilsworth, R.C. and Knottenbelt, D.C. (2005), Chorioptic mange. Equine Veterinary Education, 17: 116-117. https://doi-org.liverpool.idm.oclc.org/10.1111/j.2042-3292.2005.tb00348.x
- Paterson, S. and Coumbe, K. (2009), An open study to evaluate topical treatment of equine chorioptic mange with shampooing and lime sulphur solution. Veterinary Dermatology, 20: 623-629. https://doi-org.liverpool.idm.oclc.org/10.1111/j.1365-3164.2009.00855.x
- Curtis CF. Pilot study to investigate the efficacy of 1% selenium sulphide shampoo in the treatment of equine chorioptic mange. Veterinary Record 1999; 144: 674–5
- Littlewood JD. Chorioptic mange: successfully treatment of a case with fipronil. Equine Veterinary Education 2000; 12: 144–6.
- Rendle DI, Cottle HJ, Love S et al. Comparative study of doramectin and fipronil in the treatment of equine chorioptic mange. Veterinary Record 2007; 161: 335–8
- Mignon, Bernard & Losson, Bertrand. (2008). Dermatitis in a horse associated with the poultry mite (Dermanyssus gallinae). Veterinary dermatology. 19. 38-43. 10.1111/j.1365-3164.2007.00646.x.
- M.S. Sorrell, R.E. Fish, K.H. Taylor (2009) Pediculosis in two research ponies (Equus caballus) J Am Assoc Lab Anim Sci, 49, pp. 487-490
- Da Silva, A. S., Tonin, A. A. and Lopes, L. S. (2013) ‘Outbreak of Lice in Horses: Epidemiology, Diagnosis, and Treatment’, Journal of Equine Veterinary Science, 33(7), pp. 530–532. doi: 10.1016/j.jevs.2012.08.003.
- Paterson, S. and Orrell, S. (1995), Treatment of biting lice (Damalinia equi) in 25 horses using 1% selenium sulphide. Equine Veterinary Education, 7: 304-306. https://doi-org.liverpool.idm.oclc.org/10.1111/j.2042-3292.1995.tb01254.x
- L. Ellse, F.A. Burden, R. Wall (2014) ‘Seasonal infestation of donkeys by lice: Phenology, risk factors and management’, Veterinary Parasitology,203 (3-4), pp 303-309, https://doi.org/10.1016/j.vetpar.2014.04.012.
- Ellse, L., Burden, F. and Wall, R. (2012) ‘Pyrethroid tolerance in the chewing louse Bovicola (Werneckiella) ocellatus’, Veterinary parasitology, 188(1–2), pp. 134–139. doi: 10.1016/j.vetpar.2012.03.018.
- Reinemeyer, C.R. and Nielsen, M.K. (2014), Biology and control of Oxyuris equi. Equine Veterinary Education, 26: 584-591. https://doi-org.liverpool.idm.oclc.org/10.1111/eve.12218
- Klei TR. Helminths of the skin. In:Kahn CM, Line S, ed.The Merck veterinary manual. 8th ed. Whitehouse Station, NJ: Merck & Co Inc, 2005;736–737.
- Scott, D.W. and Manning, T.O. (1980) Equine folliculitis and furunculosis. Equine Pract. 2, 11‐32
- Scott, D.W. and Miller, W.H., Jr (2011) Equine Dermatology, W.B. Saunders, St Louis. 62. p 142.
